Gallstones: Symptoms, Causes, Risks, Treatment, Diet, & More
The gallbladder is an organ in our digestive system that is located under the liver. The gallbladder stores bile that is produced by the liver. It is a green-yellow fluid that is used for the digestion of food. The gallbladder can be affected by gallstones if the cholesterol level in your bile is at an excessive amount.
The gallbladder is an organ in our digestive system that is located under the liver. The gallbladder stores bile that is produced by the liver. It is a green-yellow fluid that is used for the digestion of food. The gallbladder can be affected by gallstones if the cholesterol level in your bile is at an excessive amount.
Gallbladder stones can be painful and, in severe cases, may even require surgical intervention to remove the stones from your body. Here is all the information regarding the symptoms, causes, risks, and treatment of gallstones that you need to know.
Symptoms
One of the first gallstones symptoms can be intense pain in the upper right part of your abdomen. It can be triggered by your dietary habits, especially if you have a lot of fried food with high-fat content. The pain from gallstones does not last for a very long time. On average, the pain lasts for a few hours each time. Apart from the pain, there are other symptoms for gallstones as well, this includes:
Vomiting
Nausea
Stomach Pain
Dark urine
Clay-coloured stool
Diarrhoea
Burping
Indigestion
Asymptomatic gallstones
Gallstones are not painful by nature; the pain is caused by the blockage of bile movement from the gallbladder caused by gallstones. Since gallstones are inherently painless, studies by the American College of Gastroenterology have shown that almost 80% of people suffer from silent gallstones. In such cases, the usual symptoms of gallstones are not experienced by the patient. They are only discovered by the doctors in abdominal X-rays or when performing abdominal surgery on the patient.
Causes
A medical study has shown 80% of gallstones are made out of cholesterol, the remaining 20% is made out of bilirubin and calcium salts. As the major part of gallstones is made out of cholesterol, people with high cholesterol levels in their blood are more susceptible to gallstones. Some of the other causes of gallstones include:
When your bile consists of plenty of Bilirubin
Bilirubin is a chemical fluid produced by the liver. Its purpose is to destroy old red blood cells from the body. Due to liver disorders and some other types of blood disorders, the liver produces excessive amounts of Bilirubin. This excessive secretion of Bilirubin causes the formation of dark brown or black gallstones that are pigmented. These gallstones are formed due to the gallbladder being unable to break down the excessive amounts of Bilirubin.
When your bile consists of excessive amounts of cholesterol
Cholesterol rich gallstones develop when the cholesterol level produced by your liver is more than what bile available in your body can dissolve. Cholesterol rich gallstones tend to be yellow in colour.
When the gallbladder is unable to empty itself leading to concentrated bile
The gallbladder is an organ that functions best when it can properly store and empty its bile contents without any hindrance. When the gallbladder cannot empty its contents of bile in an orderly fashion, it leads to the development of concentrated bile that eventually leads to the formation of gallstones.
Risks
Gallstones have many risk factors, some of which are controllable while others are uncontrollable. The controllable risk factors generally relate to a person’s diet. The uncontrollable factors delve into the person’s gender, sex, age, race, family history. These factors can’t be changed; Hence they are called the uncontrollable risk factors of gallstones.
Controllable risk factors
Having obesity or being overweight
Suffering from diabetes mellitus
Suffering from sudden weight loss in a very short period of time
Eating a high fibre diet that is fat and cholesterol heavy and also low in fibre.
Uncontrollable risk factors
Being Female
Belonging to the Native American race
Being over 40
Belonging to the Hispanic and Mexican ethnicity
Having liver disease
Gallstones can lead to different types of complications they are mentioned below:
Complications
Inflamed gallbladder: The inflammation of the gallbladder can be very painful and even cause fever. The inflammation is caused when a gallstone is created at the neck of the gallbladder. The gallstone stops the flow of bile out of your liver and causes the inflammation of the gallbladder.
Gallbladder cancer: Gallbladder cancer is a condition that affects people that have a history of gallstones. This type of cancer is highly rare, and even with a history of gallstones, the probability of being affected by gallbladder cancer remains considerably low.
Treatment
The treatment of gallstones is commonly done through surgery. However, it is possible that you might not need surgery. This is because, more often than not, gallstones do not show any symptoms or pain. People often pass their stones without feeling any pain. In case you are feeling pain from gallstones, doctors might recommend getting surgery. In rare cases, even medicinal treatment is used for curing gallstones.
Diet
For dietary practices maintaining a low fat and cholesterol diet is one of the key factors to protect yourself from the risk of gallstones. Gallstones often contain mostly cholesterol, so it is essential to maintain the cholesterol levels in your body. Avoiding food that can increase your cholesterol levels can help you keep your gallstone risk in check.
Foot Pain in Arches, Ball, Heel, Toe and Ankle Problems
Many people suffer from pain in their feet for various reasons. These reasons can be due to ageing or any underlying problem or condition that might require serious medical treatment. Nonetheless, pain in any
Many people suffer from pain in their feet for various reasons. These reasons can be due to ageing or any underlying problem or condition that might require serious medical treatment. Nonetheless, pain in any body part is something that you should monitor and get medical help for if the pain is persistent and increasing.
If you are suffering from persistent foot pain, it is important to localise the pain. When you know the location of the pain, it can help you track down the reason that might be causing the pain. Here are some of the common foot pains that people suffer from to help you identify your problem. The categorisation is done in regards to the area of the foot where the pain is located.
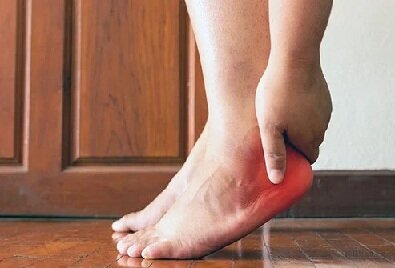
Foot Pain In Heels
Heel Spurs
Description: Heel spurs are a type of foot pain caused by the unnatural growth of the heel bone of your feet. The abnormal growth can be caused by different reasons, such as having an abnormal/peculiar step or posture. It can also be caused by physical activities such as running. Even though this condition is common, most people do not feel pain due to their heel spurs. People that have high foot arches or flat feet are more susceptible to having painful heel spurs.
Treatment: Heel spurs can be treated by wearing medically prescribed heel pads and orthotics. If you are suffering from painful heel spurs, you will need to have pain medication and get medical help to understand the severity of your issue. The doctors can also suggest medical procedures that can help you permanently solve your problem.
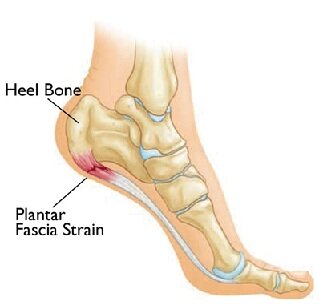
Plantar Fasciitis
Description: Plantar Fasciitis refers to pain in the tough tissues of your heel that connect the heel bone of your foot to the toes. This pain can be felt in the arch and the heel of your foot, and it affects the most in the morning when a person is getting out of bed.
Treatment: Standard treatment for this problem includes wearing shoes that have well-cushioned soles and good arch supports. You also need to adequately rest your foot and exercise using heel, and arch muscle stretches.
Foot Pain In Arch Of Foot
Bunion
Description: A bunion is an abnormal projection in the bones near the edge of your foot; it is usually located near the base of the big toe of your foot. This is a very common condition that can affect anyone. It generally affects people more as they age. It is also found in people that wear non-fitted and uncomfortable shoes over a long period of time.
Treatment: One of the first and foremost treatments for bunions include wearing properly fitted and comfortable shoes. People are often prescribed to wear shoe inserts to help them with their condition. In case your pain persists and does not reduce over a long period of time, you need proper medical care, and doctors might even suggest surgical intervention.
Claw Toe
Description: A claw toe is a serious condition where your toes either point upwards or downwards naturally and cannot be straightened. This condition is caused by various reasons such as nerve damage, alcoholism, and diabetes.
Treatment: Treatment of claw toe requires surgical intervention; however, if you are not comfortable with the notion of surgery, you can try wearing shoe inserts, avoid wearing tight shoes and high heels. You can also do stretches and exercises for your toes and toe joints.
Foot Pain In Ball Of Foot
Sesamoiditis
Description: Sesamoiditis is a condition that usually affects runners and ballet dancers. It is a form of tendinitis that affects the tendons of your foot that solely connect to two bones at the base of your big toe. This condition is caused by the injury or the inflammation of these tendons, as these tendons are called sesamoids.
Treatment: Common treatment procedures for sesamoiditis include icing the area that hurts and also wearing comfortable foot pads and comfortable shoes to reduce the pain as much as possible. If the pain does not decrease, you should get medical help where the doctors might prescribe you steroid injections.
Morton’s Neuroma
Description: Morton’s neuroma is a condition that mainly affects women who wear very high heels and tight shoes. This condition affects the tissues in between the third and fourth toes of your foot. The tissues around the nerves get thick and cause pain, numbness, or a general odd feeling in the ball of your foot.
Treatment: Common treatment procedures for Morton’s neuroma include taking pain relievers for reducing the pain in your foot. You can also use footpads inside your shoes to reduce the pressure on the nerves and reduce the pain. For treatment purposes, you should also reduce or stop wearing high heels or shoes with a very short toe compartment. If the pain does not subside over time, you need medical attention; the doctors can prescribe steroid injections and surgical procedures to treat the problem.
Early Symptoms Of COVID-19 In Children: What Parents Should Know
COVID-19 has caused the deaths of lakhs and the sufferance of even more people in India so far. The aggressive second wave of the COVID-19 virus had rattled the country to its core, with thousands of deaths every single day. The medical body of India announced the third wave of the COVID-19 virus as well.
COVID-19 has caused the deaths of lakhs and the sufferance of even more people in India so far. The aggressive second wave of the COVID-19 virus had rattled the country to its core, with thousands of deaths every single day. The medical body of India announced the third wave of the COVID-19 virus as well. It was informed that the third wave of the pandemic might largely affect children and infants. In a time like this, where the county has not yet recovered from the blow of the second wave of COVID-19, the possibility of infections among children is horrifying for parents around the country.
COVID-19 has developed more symptoms now than there were when it first appeared. These symptoms can be identified, and treatment can be ensured as soon as possible to ensure that the treatment is successful. So, here are some of the leading symptoms of COVID-19 in children that parents must know and look out for to avoid COVID-19 infection among children.
Primary Early Symptoms For COVID-19 Infection In Children
It is seriously concerning that the COVID-19 infection hides itself in children by not showing off too many symptoms on the surface. Most children affected by COVID-19 remain asymptomatic. This creates a considerable problem in identifying the infection and getting started on the treatment in the early stages. It has been noticed that in most cases, one of the parents was infected by the virus, while no symptoms of the infection were detected in the children. It was only after a test it was revealed that the children were also infected.
Here are some of the general symptoms that are common in children for the COVID-19 virus.
Cough
Fever
Breathlessness
Myalgia
Sore Throat
Diarrhea
Loss of Taste
Loss of Smell
Loose Motions
Vomiting
Nausea
Nasal Congestion
Dry Cough
Headache
Body Pain
Muscle Pain
These are some of the preliminary symptoms of COVID-19 if your child is showcasing multiple of these symptoms, especially fever with dry cough and breathlessness. The chances of COVID-19 infection are high in such cases. These are, however, not all the symptoms that you need to keep a lookout for; there are many other symptoms that, as parents, you need to look out for to maintain the safety of your children.
In some serious cases, children have been seen to suffer from ulcers in the oral cavity as a symptom of COVID infection. Even MIS, which stands for Multisystem Inflammatory Syndrome, has been noticed to be a symptom of COVID-19 infection both in children and adults. It is highly rare, but it is something that you should know.
MIS affects the patient’s kidneys, heart, lungs, brain, skin, and gastrointestinal tract. This health condition is serious, and it requires immediate medical support. You can identify MIS from these symptoms.
Diarrhea
Vomiting
Neck Pain
Fever
Low Blood Pressure
Rashes
Fatigue
Bluish Face
Breathing Problems
Abdominal Pain
Inability to walk
And Organ Inflammation
These are the symptoms that you need to keep in check to make sure your children are safe from COVID-19. The pandemic is still at large, and the future is bleak at best; in such times, it is needed to be aware of the danger at hand and the symptoms that are a part of it. For the people that are still healthy and well, it is possible to take preventive measures to save yourself, your family, and your children from the deadly virus. Here are some of the precautionary measures you can take to protect your children from COVID-19.
Preventive Measures Of COVID-19 For Children
The preventive measures of COVID are similar when it comes to children and adults. However, it is harder for children to understand the gravity of the situation and follow the protocols. But they should listen carefully to their parents, and parents especially should tactfully teach their children to wear a mask, sanitize regularly, and maintain social distance. These are the golden rules when it comes to preventive measures for COVID-19.
As vaccination is not available for children in India. It is important for the parents and every adult in the house to get vaccinated so as to protect the children from contracting the virus.
And last but not the least, it is extremely crucial to maintain cleanliness in the house with children. Cleaning the frequently touched surfaces of children is necessary also to protect them from the virus.
These are all the common symptoms and preventive measures that you need to be aware of to build a safe and hospitable environment for your children. In these challenging times, these are some of the ways that you can ensure the safety of your family and children.
Black Fungus vs. White Fungus
While the world was sufferings of from the grips of a deadly pandemic, India group and a new problem while going through its second wave of the COVID-19 virus. Throughout the country, starting from the end of April 2021, cases of black fungus and white fungus, later on, started cropping up in different parts of the country.
While the world was sufferings of from the grips of a deadly pandemic, India group and a new problem while going through its second wave of the COVID-19 virus. Throughout the country, starting from the end of April 2021, cases of black fungus and white fungus, later on, started cropping up in different parts of the country. In most cases, these fungal infections affected patients suffering from the COVID-19 virus or who w the world class company is not a very hap your family and friends and family from the family members of the day I am in thepy Birthday to you on this device in the world and the day of the year of the year ahead and have a call with you andere recently treated from the COVID-19 virus.
The cases of black fungus and white fungus are quite rare to contract; doctors all around the country informed a few reasons for the rise in cases of these fungal infections. People that suffer from diabetes were seen as people with comorbidities and more susceptible to COVID-19. Those people, when affected by COVID-19, took a massive hit in the health of their immune system.
The deteriorating condition of a person’s immune system in combination with the steroids that were used to treat their COVID-19 infection caused them to become highly susceptible to the black and white fungal infections. Now that you know the cause of their uprising, let’s look into the differences, symptoms, treatments, and preventive measures of black and white fungus.
Difference Between Black & White Fungus
| Black Fungus | White Fungus |
|---|---|
| ● Description: Black Fungus is called Mucormycosis; it is contracted when a person is exposed to the naturally found mucor mould from an open wound or burn or any other type of skin trauma. The infection is very aggressive and rapidly spreads throughout the patient's body. It usually affects the nose at first, then moves to the eyes and then the brain, causing the patient's death. | ● Description: White Fungus is a fungal infection that is caused by the candida group of organisms; it usually causes the formation of a white membrane or white discharge, and the infection resulting in that is called candidiasis. One of the leading causes for this condition is the overuse of steroids which is regularly practised nowadays for the treatment of COVID-19. The other more horrifying reason is the use of unsterile oxygen cylinders, which is also regularly needed for people suffering from COVID-19. |
| ● Symptoms: General symptoms include excessive watering and pain in the eyes, severe headaches, discolouration of the skin and tissues in the nose and cheek region of the face. There are more symptoms such as sudden toothaches, congested nose, blurred vision or loss of vision in extreme cases. Symptoms can also include swelling of the eyes and cheeks with low or high amounts of bleeding from the nose in severe cases. | ● Symptoms: This infection affects the patient in their kidneys, mouth, nail, skin, brain, and lungs. In cases where the infection reaches the lungs and the blood and creates a systemic infection, the chances of the patient’s survival become close to none. The general symptoms include symptoms of pneumonia and low oxygen levels, along with lesions on the skin oozing white discharge and whitish patches in the oral cavity. |
| ● Treatment: This is an extremely serious condition that requires surgical removal of all the affected tissues. In many cases, when the infection reaches the eyes of a patient, the doctors have had to remove their eyes in order to save their lives. Patient's also have had to remove their upper jaws to treat themselves from this condition. It is not possible to treat this condition through medicines alone, and in most cases, surgical intervention is required for the treatment. | ● Treatment: Treatment of the white fungus infection does not require surgical intervention and can be treated with oral and topical medication. Oral treatment options generally include fluconazole or itraconazole. When the infection reaches the oral cavity or genital regions, topical application of medically prescribed ointments and creams are required. |
| ● Prevention: One of the first and most important preventive measures for the black fungus is to keep your blood sugar levels under control. Other than that, it is also imperative to be under constant medical supervision when you are on steroidal treatment for COVID-19 or other ailments. In some cases, patients also require a four to six-week intravenous antifungal procedure to prevent this condition from affecting them. | ● Prevention: This condition is caused by unsterilised medical equipment such as ventilators and oxygen cylinders. It is essential to properly clean and sterilise such equipment before providing it to patients. Patients themselves have little to no say in their contraction of the white fungus infection. So, healthcare providers need to do an adequate job to ensure patients are not suffering from such infections. |
Which Skin Condition Is Common In Older Adults?
Ageing is not directly related to skin conditions, but our skin becomes thinner, less oily, and less elastic as we age. These factors make our skin prone to skin diseases. The rate of ageing for your skin depends on various factors such as lifestyle, personal habits like smoking, heredity, and diet. As you age, one of the biggest causes of skin damage is sun exposure.
Ageing is not directly related to skin conditions, but our skin becomes thinner, less oily, and less elastic as we age. These factors make our skin prone to skin diseases. The rate of ageing for your skin depends on various factors such as lifestyle, personal habits like smoking, heredity, and diet. As you age, one of the biggest causes of skin damage is sun exposure. The UV radiation from the sun causes the skin to sag, stretch, and become blotchy.
As older people are more susceptible to skin diseases, it is necessary to check your skin for any signs of rashes or other conditions to keep your skin healthy and safe. Skin conditions that affect you in older ages take longer to heal and generally do not go away without treatment.
So, let’s look at some of the common skin conditions that affect older people and their treatment and preventive measures.
4 Skin Conditions That Affect Older Adults
1. Senile Purpura
Description: Senile Purpura is a type of skin condition that generally affects older adults. As the skin becomes thinner over time, so do the blood vessels. Thinner blood vessels are more prone to disruption and bruising; this results in bruise marks commonly found on the forearms.
Symptoms: Bruise marks on different parts of the body, especially forearms. This condition does not have any links to any vitamin deficiency or bleeding disorders. However, seeking treatment is in your best interest.
Treatment: Treatment includes medically prescribed topical retinoids for improving the thickness of your skin; this helps reduce the further effects of ageing on your skin. Generally, treatment for this condition is cosmetic as it does not pose any severe harm to your health.
Prevention: Best prevention methods include using sunscreen and reducing exposure to the sun as much as possible. It can help your skin avoid any further damage from the effect of UV radiation from the sun.
2. Xerosis
Description: Xerosis is a skin condition caused by the lack of oil content in the skin. Dry skin with a lack of oil content is common in older adults who commonly suffer from this condition. The skin appears dry and flaky and generally affects areas like the lower back, arms, and shins.
Symptoms: Scaly and flaky skin in a netlike pattern in areas such as limbs, shins, lower back. It can also appear as significant red round patches, red scaly fissures.
Treatment: Improving your skin hygiene and using a thick moisturiser can help improve the symptoms of this condition. You can also use a humidifier to improve the dryness of your skin. If your condition does not improve by following these steps, you must take medical advice.
Prevention: Dietary changes such as reducing the amount of caffeine and alcohol intake can also help you prevent conditions like xerosis. Also, limiting your exposure to water by reducing the time of your showers can help.
3. Senile Freckles
Description: Senile freckles are one of the facial skin diseases that affect the elderly. This condition is caused due to the cumulative skin damage caused by exposure to the sun over the years. This condition differentiates itself from freckles as the spots caused by this condition are larger and irregularly shaped in comparison to freckles.
Symptoms: Large Brown spots on the face that resemble freckles. If the freckles are growing or becoming thicker, you should get medical help as it can be signs of cancerous growth.
Treatment: This condition can be treated medically or by surgical processes such as freezing the freckles and electrosurgery. Using certain chemical peels and skin lightening creams.
Prevention: Using sunscreen with an SPF value higher than 50 and limiting your skin exposure to the sun. You should also wear clothes that cover your skin and wide brim hats to prevent this condition.
4. Stasis Dermatitis
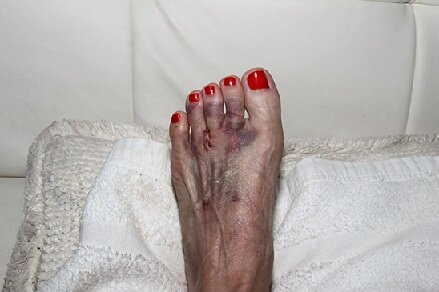
Description: Stasis Dermatitis is a type of skin condition that usually affects areas such as the legs. This condition is caused due to poor blood circulation in older adults. It is necessary to pursue treatment for this condition as it can have serious health hazards if left untreated.
Symptoms: Rashes usually in areas such as the ankles, legs, and feet. Symptoms also include discolouration of the skin, itching, and thickened skin.
Treatment: Medically prescribed topical creams can help reduce the symptoms. You can also use compression stockings for the treatment of this condition.
Prevention: You should avoid sitting or standing for long hours; propping up your feet while sitting can also be beneficial.
As we age, the immunity powers of our body reduce and cause different skin conditions to appear. Some of these conditions can be indicators of severe health issues and should be medically checked and treated at the earliest. This way, you can avoid any type of skin condition in the future and have healthy and supple skin throughout your life.
What Causes Red Itchy Bumps On The Skin?
Do you have red itchy bumps all over your skin for no reason? The red itchy bumps are often referred to as rashes, and there can be an ample number of reasons behind them. While some of us have it just due to the change in weather, others might get blisters or those bumps as an allergic reaction of the body.
Do you have red itchy bumps all over your skin for no reason? The red itchy bumps are often referred to as rashes, and there can be an ample number of reasons behind them. While some of us have it just due to the change in weather, others might get blisters or those bumps as an allergic reaction of the body.
Besides, there are several types of rashes that affect the skin in different parts of the body. There is a varied range of factors that can cause itchy bumps on the skin. Some of them are:
Exposure to environmental allergens
Certain diseases such as measles or chickenpox
Allergic reaction to medications, food or certain metal objects such as nickel earrings
Infections such as ringworm
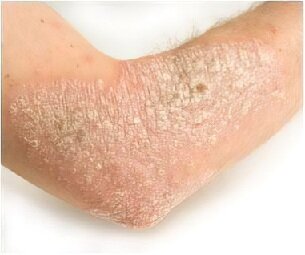
Chronic troubles such as psoriasis
Let’s dive in deeper and find out about some of it in detail.
1. Fifth disease
Description: Anyone with a weak immune system can get affected with the fifth disease. However, pregnant women or kids are more vulnerable to getting affected by it even though the effects are not really that severe. It causes red rashes on the legs, cheeks and different other parts of the body.
Symptom: The symptoms are quite similar to that of the common flu. However,
it usually includes itchy rashes, headache, fatigue, sore throat and several other symptoms.
Treatment: There is no such treatment for this disease as the effects are quite mild. However, it is best to take adequate rest and to drink lots of healthy fluids for getting healed soon.
Prevention: The fifth disease is contagious and is often spread from respiratory secretions like sputum or saliva. That is why it gets transmitted easily, as it is highly contagious. Therefore, the only way of prevention is to maintain distance from the person suffering from it.
2. Atopic dermatitis
Description: Atopic dermatitis or eczema is a skin disease that leads to itchy, cracked skin and inflammation. There are several kinds of eczema, among which some lead to blisters as well.
Symptoms: The symptoms basically depend on the age of the affected person. Atopic dermatitis often results in dry patches on the skin, which are intensely itchy. Open sores or skin flushing are also two common symptoms of this skin condition.
Treatment: The only way to treat these skin issues is by treating the affected skin and by preventing it from further infections.
Prevention: Wear comfortable cotton garments and avoid wearing clothes made of harsh and rough materials. Make sure to moisturize the skin after certain intervals.
3. Skin Allergy or Allergic contact dermatitis
Description: While some of us are allergic to certain medications or food products, others are allergic to various types of objects. There are a variety of everyday things which can lead to skin allergy, i.e., itchy red bumps on the body.
Symptoms: Itchy rashes on the face or arms are the most notable symptoms. Besides, the symptoms generally develop within a day, but the after effect takes about a week to go away.
Treatment: There are several medications for easing the effect of these allergies. But calamine lotions or oatmeal baths quite often reduces the itching and heals the affected areas swiftly.
Prevention: The only option to prevent your body from getting triggered by the allergens is by avoiding consuming certain foods, medications or reducing the usage of objects that might lead to allergies on your skin.
4. Fungal Infection
Description: From athlete’s foot, ringworm to Jock itch, all of these fungal infections are caused by a fungus that survives in warm and moist areas of the body such as the underarms, toes and groin.
Symptoms: The symptoms depend solely on which part of the body it has affected. While some might be itchy red patches on the skin, the other ones might also give a burning sensation besides an intense itchy feeling.
Treatment: Consulting a dermatologist and following his advice is the best way to tackle these infections. There are a number of antifungal medications and medicated creams that are used for the healing of the affected areas.
Prevention: It is a contagious disease and often spreads when you come in touch with an infected individual, pet or an infected area of an object. The only way of prevention is to avoid using the same towels or other belongings of an infected person.
There can be many reasons why itchy bumps suddenly appear on your skin. However, maintaining proper hygiene and avoiding coming in contact with an infected individual are some of the best ways to prevent this unwelcoming trouble.
Skin Rash: COVID-19, Types, Causes, Treatment & Prevention
Skin rashes are an uncommon symptom of COVID-19. However, in asymptomatic young adult patients, the symptom of skin rashes has been found more commonly than others. Skin rashes are not yet listed as official symptoms of the COVID-19 virus, but certain skin rashes could be an indicator that you might be affected by COVID-19.
Skin rashes are an uncommon symptom of COVID-19. However, in asymptomatic young adult patients, the symptom of skin rashes has been found more commonly than others. Skin rashes are not yet listed as official symptoms of the COVID-19 virus, but certain skin rashes could be an indicator that you might be affected by COVID-19.
If a patient is suffering from fever symptoms and starts getting rashes on their skin, the chances of the patient suffering from COVID-19 increase. They must immediately get tested to see if they have contracted the COVID-19 virus. Some rashes have been commonly found to be affecting people suffering from COVID-19.
Let us discuss their types, causes, treatments, and prevention below.
5 Skin Rashes That Can Be Symptoms Of The Covid-19 Virus
1. COVID Digits
Description: COVID digits refer to red and purple rashes on the fingers and toes of a patient. These rashes were common in the colder months of the year, but after they affected people in the warm months too. It was connected to be a symptom for COVID-19. However, officially it is not listed as a COVID-19 symptom.
Symptoms: Inflammation on the fingers and toes of patients with red and purple rashes that cause soreness. These rashes are not known to cause itchiness. If they are accompanied by fever, it can increase the possibility of COVID-19 infection.
Treatment: As this rash is related to COVID-19, it is essential to get tested for the virus if you show any other symptoms along with the rashes. For the rashes, you can use topical nitroglycerin gels.
Prevention: Avoid over-exposure to cold temperatures. Keep your hands, face, and feet warm and dry. Be sure to wear a mask, sanitise regularly, and maintain social distancing.
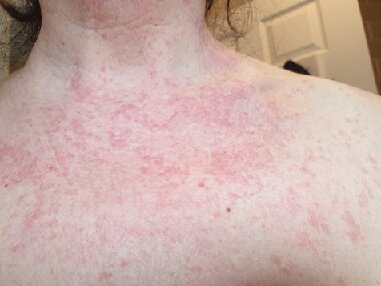
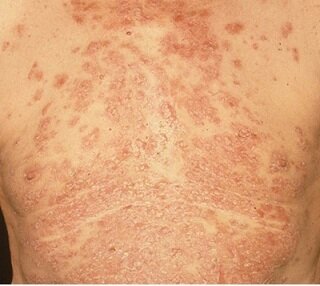
2. Eczema on Neck and Exposed Chest Regions
Description: Neck and exposed chest eczema has been linked to patients suffering from or recovering from COVID. This rash appears on the patient's neck and chest area that is exposed to sunlight. These rashes are pink in appearance and itchy and can stay for an extended period.
Symptoms: Very pink rashes on the neck and exposed chest regions in direct contact with sunlight. The rashes are very itchy and cause severe irritation.
Treatment: The best way to treat this condition is to avoid using soaps and other irritants. You can also use some medically prescribed ointment and gels to provide comfort from the itching and irritation.
Prevention: Do not use harsh soaps, detergents, and solvents. Avoid wearing scratchy fabric like wool and moisturise regularly.
3. Oral Rashes
Description: Oral Rashes are found on the lips of people suffering from or recovering from COVID-19. These rashes can be found on the patient's lips, and it causes the lips to be sore. Oral rashes are uncommon and cannot always be linked with COVID-19.
Symptoms: Soreness and rashes on the lips, dry and scaly lips. These rashes can also cause soreness inside your mouth.
Treatment: For pain relief, you can use medicines such as Tylenol. Also, try gargling with salt and water.
Prevention: Using proper dental hygiene is essential for protection against oral rashes. You should also consider not consuming very hot foods or drinks.
4. Pityriasis Rosea
Description: This type of rash can be caused due to viral infection, although it has not yet been completely confirmed. They appear either on your chest, abdomen, or back.
Symptoms: This rash often starts out as a large spot on your abdomen, chest, or back followed by smaller lesions.
Treatment: These rashes can heal on their own in their own time, although you can use certain antihistamines and antiviral drugs to get rid of this rash quickly.
Prevention: This rash does not have any clear prevention steps as the cause for this rash is not yet fully understood. The best call of action is to maintain proper hygiene and follow COVID appropriate behaviour.
5. Hives
Description: Hives or urticaria is a type of rash that develops rapidly and can affect any part of the body. In the case of a COVID-19 patient, these rashes can show when the virus shortly infects the person. However, this rash is more long-term for people healing from the virus and is no longer contagious.
Symptoms: Appears on any part of the body and is intensely itchy. It can also cause swelling in certain areas of the body.
Treatment: These rashes can go away as quickly as a few hours on their own. In case the rashes do not go away, you can opt for antihistamine medication.
Prevention: It is crucial to maintain proper skin hygiene to avoid these rashes. Also, avoid using hot water showers to prevent hives.
Skin rashes are not automatically linked to COVID-19. However, the rashes mentioned above are commonly found in people either affected or healing from COVID-19. Some of these rashes can signify that you are affected by the virus, even if you are asymptomatic. So, it is essential to take these cues seriously and get yourself tested when required.
How Do I Identify A Rash?
Rashes are a type of skin disease that is defined as a general outbreak of skin lesions. Rashes differ drastically from one another in terms of appearance. The appearance and its symptoms are some of the main ways to identify a rash.
Rashes are a type of skin disease that is defined as a general outbreak of skin lesions. Rashes differ drastically from one another in terms of appearance. The appearance and its symptoms are some of the main ways to identify a rash. Rashes are generally non-lethal, but they should not be left untreated. So, you must identify rashes by their symptoms and go for treatment with either over the counter medication or proper dermatological help.
Rashes can be caused by various factors such as contact dermatitis, allergic reaction to food and drugs, fungal, viral, and other types of infections. Rashes are generally distinguished based on their appearance. Some of the factors considered for determining different rashes are dryness or moisty, bumpy or smooth, blistered or cracked, and if they are painful, itchy or both. In rare cases, it has been noticed that rashes also change colour in their course of infection.
Now that you know the different factors used for differentiating between rashes let’s find out how you can identify a rash and what steps you can take to cure them.
5 Types Of Rashes You Can Identify At Home
1. Fifth Disease
Description: The fifth disease is a type of rash that affects children especially. It affects the cheeks commonly with circular bright red rashes on them.
Symptoms: Along with the rashes on the cheeks, it can also cause fever, diarrhoea, nausea, and fatigue.
Treatment: These rashes are painful and more so because they commonly affect children. These rashes go away on their own in due time, but pain-relieving medication might be required to alleviate the pain.
Prevention: Maintaining proper hygiene with regular washing of hands with soap and water. Covering your face when sneezing or coughing and not touching your eyes, nose, and mouth in public.
2. Rosacea
Description: Rosacea is a chronic skin disease that infects a person for a long time. This rash goes through phases of disappearance and relapse. Rosacea also has four different subtypes, all of which have varying symptoms.
Symptoms: Rosacea comes with facial redness with red bumps on the skin and facial flushing, along with skin dryness and sensitivity.
Treatment: This skin condition is serious and should not be left untreated as it tends to get more serious over time. The go-to medication for this disease is antibiotics and anti-acne medication.
Prevention: Use proper sun protection by covering up and using sunscreen. You should also reduce your exposure to high temperatures.
3. Ringworm
Description: Ringworms are scaly in nature, and they are circular in shape with raised borders. The skin in the middle seems normal, and only the raised edges seem to spread outward. Ringworms can be very itchy in nature.
Symptoms: Circular rashes on the skin with raised red edges that are highly irritating and itchy.
Treatment: Ringworms are a type of fungal infection that does not go away on its own. You need to use treatment over the counter or medically prescribed anti-fungal medication.
Prevention: As it is a fungal infection, the best way to prevent it is to make sure you follow proper skin hygiene and keep your skin dry. Make sure to wear clean clothes and change your underwear every day.
4. Allergic Eczema
Description: Allergic eczema resembles a burn with blisters, scaly, and raw skin that ooze or become crusty. They are usually noticed on the hands and forearms of a person and are red and itchy in nature.
Symptoms: Scaly, raw, and itchy skin forms blisters and ooze out pus or becomes crusty on top. In terms of appearance, it may resemble a burn.
Treatment: Medical treatment for this condition includes using both over the counter and prescribed medications such as hydrocortisone cream to reduce the itching. You should also moisturize the affected area with fragrance-free moisturizers.
Prevention: Moisturizing is the key to preventing this condition. You should also avoid hot places that make you sweat a lot.
5. Psoriasis
Description: Psoriasis usually affects areas such as the knees, elbows, and lower back regions. It involves the skin turning silvery in colour, with very defined patches appearing on the skin. This infection also causes the affected skin to become scaly.
Symptoms: Itchy patches of skin that turn silvery in colour. This condition can also be asymptomatic, which means the appearance changes without any itching.
Treatment: Medical treatment for this condition includes using topical ointments and gels for relieving the symptoms. The treatment aims to reduce the cells from growing too fast.
Prevention: Properly moisturizing your skin is a must to prevent psoriasis. You should also maintain proper care and hygiene of your skin and scalp.
Skin diseases are common, and everyone suffers from them from time to time. The key is to identify it properly and treat it as soon as possible. If you are unable to identify the rash at home, be sure to get medical help. Untreated skin diseases can be problematic for you, so do not take them very lightly.
Skin Rash: Skin Disorders: Pictures, Causes, Symptoms, Treatments
Skin disorders are prevalent among people of all ages and races. As the skin is the largest organ of your body, it is exposed to different elements that can cause problems such as rashes, allergies, and skin disorders.
Skin disorders are prevalent among people of all ages and races. As the skin is the largest organ of your body, it is exposed to different elements that can cause problems such as rashes, allergies, and skin disorders. Skin disorders often share similar symptoms, which is why it is hard to identify from which condition you are suffering.
Most skin disorders are not severe, and they do not pose any real threat to your health and well-being in the long run. However, some disorders have the potential of becoming harmful to your health over time. So it is essential that you keep a check on your problems and get them treated as soon as possible.
Skin disorders can be irritable, sore, itchy and hard to get rid of, but it is essential that you identify the type of skin disorder you have for it to be treated soon. Delaying treatment might cause the affected area to spread further, and the skin disease can become even tougher to heal. So, let’s take a look at some common skin disorders and how you can treat and prevent them.
4 Common Skin Disorders And How To Treat Them
1. Seborrheic Dermatitis
● Description: This condition is common for babies, but it can affect adults as well. It is usually harmless and can go away on its own in due time. In babies, this condition is known as a ‘cradle cap’. In adults, this condition can affect any part of the body, and the condition will be prone to appearance and disappearance throughout the patient’s life.
● Symptoms: For babies, the symptoms include scaly and greasy skin, especially on the scalp. For adults, the symptoms are different as the skin tends to become swollen and reddish in colour with a greasy look.
● Treatment: This condition requires continuous treatment in the form of medicated soaps and shampoos. You may also need to use medically prescribed anti-fungal and anti-inflammatory medications.
2. Moles
● Description: Moles are a very common skin condition that appears when skin cells gather up with tissues surrounding the area. Moles can appear in your body at any time during your lifetime. In general, moles are harmless, but they should be checked out if they grow abnormally or change colour.
● Symptoms: There are no such symptoms when it comes to moles. Moles appear as a projection on your skin, generally blackish or brownish in colour. They can appear randomly without any prior symptoms.
● Treatment: Moles are essentially harmless in most cases, and they do not require medical treatment. If you are not happy with the moles on your body and want to treat them, the treatment process is surgically removing the mole.
3. Melanoma
● Description: Melanoma is a condition that is directly linked to moles. It is a form of serious skin cancer that can be fatal if not treated properly. Melanoma is the consequence for which moles need to keep in check. This condition can affect children and adults both.
● Symptoms: Melanoma can be identified when you notice any irregularly shaped mole on your body. You should also be alarmed if any moles are coloured in an uneven manner.
● Treatment: Melanoma is a type of skin cancer. The treatment process includes chemotherapy and radiation therapy. Melanoma can be treated if it is diagnosed early on; in the later stages, it can be fatal, so early diagnosis is a necessity.
4. Lupus
● Description: Lupus is a serious skin disorder that affects the immune system of the body. This condition is highly complex and varies greatly from person to person. The skin rashes that appear from lupus are not irritating, but it affects your body in other ways such as fever, headaches, and pain in the joints.
● Symptoms: Red patches of skin that are ring-shaped and sunburn-like spots on the nose and cheek are some of the most common symptoms of lupus. If the rashes mentioned are followed by bouts of fever, fatigue, and headaches, it can be a significant symptom that you are suffering from lupus.
● Treatment: Lupus is an incurable condition that cannot be fully treated. Treatment for this condition focuses on improving the lifestyle of the affected by controlling the flare ups experienced by the patient. Steroids and anti-inflammatory drugs can be used as a medication for controlling this condition.
Skin disorders are common, but they require certain lifestyle and personal hygiene changes for the best course of treatment. More often than not, skin disorders are easier to treat when they are diagnosed early on. Still, in later stages of diagnosis, some skin disorders can become untreatable as well as fatal. So, it is crucial for you to pay close attention to your skin health to avoid such diseases.
What Are Rare Skin Diseases?
Be it an abnormal-looking red bump on your skin or sudden itchiness at certain portions, issues related to skin conditions are quite common among people of all ages. While most complications regarding our skin are treatable and do not really require any such attention, there are a handful of other rare ones which demand immediate medical advice. In severe cases, these conditions might not be curable as well.
Be it an abnormal-looking red bump on your skin or sudden itchiness at certain portions, issues related to skin conditions are quite common among people of all ages. While most complications regarding our skin are treatable and do not really require any such attention, there are a handful of other rare ones which demand immediate medical advice. In severe cases, these conditions might not be curable as well.
There are many skin diseases that are incredibly rare and affect only hundreds among millions of people. It is still crucial to know the details to stay informed regarding the symptoms and get yourself treated in case you see the symptoms appear on yourself. Read ahead to learn about the vital details of some rare skin diseases.
4 Rare Skin Diseases For You To Know
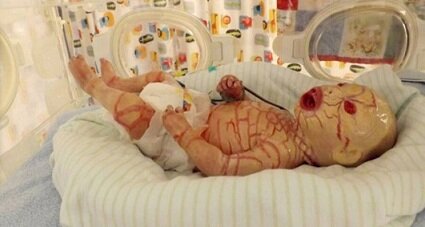
1. Harlequin ichthyosis
Description: This is a genetic disorder that often leads to the thickening of the skin at various parts of the body in newborns.
Symptoms: Infants born with this rare skin condition often have deep and shiny patches or plates of skin and thick erythematous fissures separating the layers of the plates. Other symptoms often include Eclabium, dehydration, severe ectropion, etc.
Treatment: Even though there is no such cure for this disease, you should still contact your dermatologist and follow their suggestions. In most cases, the doctors prescribe antibiotics for protecting the firm skin from causing further infection.
Prevention: As stated earlier, Harlequin ichthyosis is passed on to the next generation through autosomal recessive genes. The only way to know whether you are a carrier or not is by consulting with a genetic counsellor before conceiving. Besides, the newborn will have this rare skin disorder only if both the parents pass down the gene and not the other way round.
2. Morgellons
Description: This skin disease is often referred to as a delusional disorder. The person suffering from it often believes that foreign particles or insects are crawling inside or coming out of broken skin. Morgellons is usually misunderstood as a psychiatric disorder.
Symptoms: The primal symptom of this disease is skin rashes with thread-like coloured fibres coming out of the skin. A crawling sensation and intense itching in the affected area are also significant symptoms of this rare skin disorder.
Treatment: Based on the underlying cause of the disorder, it is treated in two different ways. In case of bacterial infections, the treatment procedure often includes a round of antibiotics consumption. The Morgellons are quite often treated with antipsychotic medications as well. However, there is no such proper treatment of this disease yet. All of the medications are prescribed just to ease the troubles for the time being.
Prevention: Morgellons is a poorly understood disease that does not have any such permanent cure options. Hence, there aren’t any ways to prevent it from affecting you. However, it is highly recommended to consult a doctor as soon as you notice open wounds on your skin without any cause and also if you experience tiredness and joint/muscle pain quite often.
3. Hidradenitis Suppurativa
Description: This skin condition often leads to bumps on different parts of the body, which is quite painful. It occurs mainly during the time of puberty and is more common in females than males.
Symptoms: One of the main symptoms of this skin disease is breakouts which look quite alike to a pimple. Some other symptoms of Hidradenitis Suppurativa also include painful and delicate nodules.
Treatment: Treatment varies based on the seriousness of the case, the modes of treatment vary from person to person. Both medication and surgery are equally fruitful options for this rare skin disease.
Prevention: Some of the most effective ways to avoid this skin trouble is by achieving a healthy body weight, opting to take warm baths and avoiding smoking habits.
4. Pemphigus
Description: This autoimmune skin condition leads to sores and blisters in the throat, mouth or in the genital area. Even though it is caused mainly to older adults, it can also affect people at any age, but the chances increase with ageing.
Symptoms: Pemphigus occurs in various types, and it depends solely on the place where it is affecting. The primary symptoms are blisters followed by fatigue, nail problems and burning sensations.
Treatment: Similar to several other rare skin diseases, there are no permanent treatment options for Pemphigus. However, dermatologists often treat the symptoms and go ahead with the treatment in order to stop the further spread of the infection.
Prevention: The cause of Pemphigus is yet to be found, and hence, there is no way you can take adequate prevention for this skin condition.
If you are concerned about the health and well-being of your skin, it is best to get medical advice from a dermatologist to find the root cause of the troubles you are facing. Most of the rare skin diseases are inherited and often have a genetic link. That is why there are no proper modes of prevention for most of them to date.
Common Rashes: Types, Symptoms, Treatments, & More
Are you facing itchiness, redness, bumps, and irritation on your skin? Chances are it could be a rash on your skin that is causing it. As the skin is the largest organ of the body, it is susceptible to different types of rashes and other skin diseases.
Are you facing itchiness, redness, bumps, and irritation on your skin? Chances are it could be a rash on your skin that is causing it. As the skin is the largest organ of the body, it is susceptible to different types of rashes and other skin diseases. There are different types of rashes, all of which can cause a considerable amount of discomfort for the person suffering from it.
It is tough to get rid of any rashes, no matter which type it is. The wisest decision is to identify the skin condition as soon as you notice it so that it could be treated and cured immediately. Let us discuss all the details about identifying and treating some of the most commonly found skin rashes below.
5 Common Types of Rashes and Their Treatment
1. Ringworm
Description: One of the most common skin conditions or infections found in people is ringworm. It is caused by a fungus which also causes another skin condition known as athlete’s foot. Ringworm gets its name from the circular shape it forms on the skin, often becoming red and cracked.
Symptoms: This type of skin rash is very itchy in nature and causes circular red areas on the skin in the affected areas. It can cause loss of hair, too, if it forms on the scalp.
Treatment: The best way to treat this type of infection is to take oral medications as prescribed by your doctor. Anti-fungal creams can also help you treat this skin rash, but be sure to consult your dermatologist before.
Prevention: This skin rash is contagious and can be caused by coming in touch with a person or surface that might contain this fungus. Avoid it by drying the groin area, skin folds and feet well.
2. Eczema
Description: Eczema is an umbrella term used for various types of skin conditions that cause flaky, red, dry and crusty skin due to lack of moisture. It usually forms on places like elbows, knees, hands and feet.
Symptoms: Extremely itchy affected area. Other symptoms include dry, red and flaky patches of skin.
Treatment: If you are showing any symptoms of eczema, you should immediately consult with your dermatologist. They can prescribe you anti-itch lotions, anti-fungal medicated soaps, fragrance-free, and non-dyed soaps that can help you cure the affected area.
Prevention: You should avoid taking long and hot showers. You can apply moisturisers while your skin is still damp from the shower, as it will help the moisturiser penetrate through the skin quickly.
3. Acne
Description: Acne is the most common type of skin condition occurring among teenagers and adults worldwide. It is characterised by red bumps or pimples on the forehead, face, chest and shoulders. It is caused by excess accumulation of oil, sebum, bacteria, and dead skin cells in the pores of your skin.
Symptoms: Pimple-like red bumps often appearing along with blackheads, whiteheads and cysts. It can sometimes be itchy too.
Treatment: It is wise to consult with your dermatologist, who might provide you with prescription medications for your acne, depending on the severity and your age. Medical methods such as chemical peels can also be used to treat your acne to remove the top layer of your skin.
Prevention: Some of the most common ways you can prevent acne are by washing your face regularly with a gentle cleanser and using a moisturiser. Keeping your hands from touching your face often also helps with acne prevention.
4. Psoriasis
Description: Psoriasis is defined as discoloured, thick, sore and dry patches of flaky skin. It is sometimes silver and flaky in nature which causes plaques that might appear on places like the face, palms, knees, elbows, back and feet.
Symptoms: Uneven raised plaques of skin, soreness, itchiness and a burning sensation.
Treatment: Psoriasis cannot be totally cured, but you can reduce it by consulting with a dermatologist and getting a prescription or over-the-counter medication.
Prevention: If you happen to have psoriasis in your genetics, you can keep it at bay by taking regular showers, moisturising your skin and getting sunlight regularly.
5. Hives
Description: Hives are defined as uneven, raised, itchy welts that can be found on your skin. It is pink, red or flesh-coloured, and it can be caused by an allergic reaction from medication or food.
Symptoms: Pinkish, red or flesh coloured welts that suddenly appear on your skin.
Treatment: Get the type of hives you have, identified by your dermatologist and get prescribed antihistamines. Avoid using hot water for a shower that might irritate hives.
Prevention: Wear loose-fitted clothes and avoid humid areas.
Ending Note
It is advised to get your skin conditions treated immediately before it spreads even more and becomes uncontrollable. So, consider getting medical help if you are showing signs of any of the above-mentioned skin diseases.
Child Vaccination Chart
Vaccination is considered to be one of the greatest breakthroughs in the history of medical science. Vaccines are the most effective and trusted way to safeguard your children from the worst of contagious and deadly diseases.
Vaccination is considered to be one of the greatest breakthroughs in the history of medical science. Vaccines are the most effective and trusted way to safeguard your children from the worst of contagious and deadly diseases.
A child’s immunity is very low when it is born and until the age of 12 years, they are highly vulnerable to contract severe bacterial and viral diseases. Certain diseases like hepatitis, HVP, diphtheria and rotavirus, can prove to be fatal for your child. However, these diseases are vaccine-preventable and once your child is immunized, there is a reduced possibility for your child to contract the disease. While the possibility cannot be completely ruled out, it can still prevent your child from dire consequences and serious complications. Timely vaccination ensures that your baby develops at least 90 percent immunity against the deadly and contagious diseases. Being a responsible parent, it calls for you to follow the child vaccinations schedule strictly, to ensure your child’s safety.
The following chart will act as a ready reckoner for you to follow strictly without missing out the timelines.
| Age | Vaccines |
| At Birth | BCG vaccine for tuberculosis OPV vaccine for polio Hepatitis B vaccine |
| 6-8 weeks | DTaP/DTwP- Diphtheria, Tetanus and Pertussis vaccine Hib- Haemophilus influenzae type B vaccine, Rotavirus, IPV- Injectable Polio Vaccine, Hep B-Hepatitis B Vaccine |
| 10-16 weeks | DTaP/DTwP-Diphtheria, Tetanus and Pertussis, Hib-Haemophilus influenzae type B vaccine, Rotavirus, IPV-Injectable Polio Vaccine |
| 14-24 weeks | DTaP/DTwP-Diphtheria, Tetanus and Pertussis, Hib-Haemophilus influenzae type B vaccine, Rotavirus, IPV-Injectable Polio Vaccine |
| 6 months | OPV-Oral Polio Vaccine, Hep B-hepatitis B vaccine |
| 9 months | OPV-Oral Polio Vaccine, Measles, MMR-Measles, Mumps and Rubella vaccine |
| 9-12 months | Typhoid CV-typhoid conjugate vaccine |
| 12 months | Hep A-Hepatitis A vaccine |
| 15 months | PCV-Pneumococcal conjugate vaccine Booster, MMR-Measles, Mumps and Rubella vaccine |
| 16-18 months | IPV-Injectable, Polio Vaccine, Hib-Haemophilus influenzae type B vaccine, DTaP/DTwP-Diphtheria, Tetanus and Pertussis |
| 18 months | Hep A-Hepatitis A vaccine |
| 2 years | Typhoid Booster |
| 4-6 years | OPV-Oral Polio Vaccine, Typhoid Booster, DTaP/DTwP-Diphtheria, Tetanus and Pertussis Booster |
| 9-15 years (girls) | HPV- Human papillomavirus |
| 10-12 years | Tdap/ Td-Tetanus, Diphtheria and Pertussis vaccine |
Post vaccination care of your child
Vaccines usually contain the dead or inactivated agent, bacteria or virus, associated with the disease, and they help build antibodies inside the body which are strong enough to fight the infection. Post-vaccination care of your child is extremely important because certain mild reactions are very common after vaccination. The reactions basically are a result of the child’s body working harder to make antibodies. The most prominent symptoms noticed after vaccination are:
● Redness at the site of injection
● Swelling at the site of injection
● Low-grade fever
● Trouble in falling asleep due to pain
It is very important to comfort your baby during and after vaccination. Parents should stay nearby so as to calm your baby during the injection. If there is too much pain or redness on the injection site, you can use a numbing cream, to soothe your baby. Immediately after the injection shot is given, gently rub your child’s skin because a light massage can help dampen the pain of the injection.
Generally, before the child turns 2, he has tolerated more than 20 shots of injection. You can also ask your doctor if there are combination vaccines available. In this, vaccinations for several diseases are combined into one shot so that the number of injections for your child are reduced. These include tetanus, diphtheria, and acellular pertussis (Dtap) vaccine, which are combined with the polio and hepatitis B vaccines, or the polio and haemophilus influenzae type b (Hib) vaccines.